Global Maternal Mortality Projections by Urban Rural Locationand Education Level: A Simulation-Based Analysis
Abstract
Background
Maternal mortality remains a challenge in global health, with well-known disparities across countries. However, less is known about disparities in maternal health by subgroups within countries. The aim of this study is to estimate maternal health indicators for subgroups of women within each country.
Methods
In this simulation-based analysis, we used the empirically calibrated Global Maternal Health (GMatH) microsimulation model to estimate a range of maternal health indicators by subgroup (urban/rural location and level of education) for 200 countries/territories from 1990 to 2050. Education levels were defined as low (less than primary), middle (less than secondary), and high (completed secondary or higher). The model simulates the reproductive lifecycle of each woman, accounting for individual-level factors such as family planning preferences, biological factors (e.g., anemia), and history of maternal complications, and how these factors vary by subgroup. We also estimated the impact of scaling up women’s education on projected maternal health outcomes compared to clinical and health system-focused interventions.
Findings
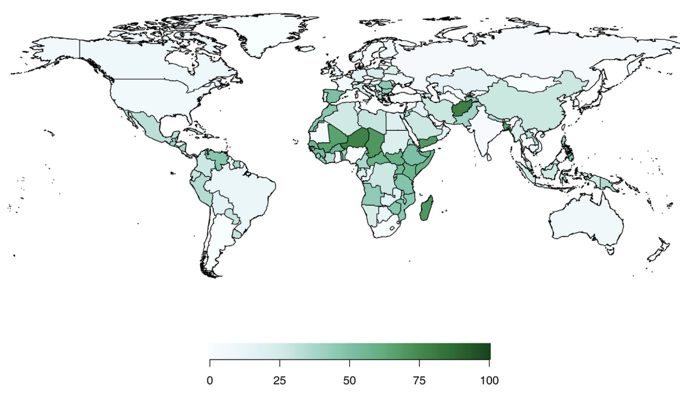
We find large subgroup differences in maternal health outcomes, with an estimated global maternal mortality ratio (MMR) in 2022 of 292 (95% UI 250–341) for rural women and 100 (95% UI 84–116) for urban women, and 536 (95% UI 450–594), 143 (95% UI 117–174), and 85 (95% UI 67–108) for low, middle, and high education levels, respectively. Ensuring all women complete secondary school is associated with a large impact on the projected global MMR in 2030 (97 [95% UI 76–120]) compared to current trends (167 [95% UI 142–188]), with especially large improvements in countries such as Afghanistan, Chad, Madagascar, Niger, and Yemen.
Interpretation
Substantial subgroup disparities present a challenge for global maternal health and health equity. Outcomes are especially poor for rural women with low education, highlighting the need to ensure that policy interventions adequately address barriers to care in rural areas, and the importance of investing in social determinants of health, such as women’s education, in addition to health system interventions to improve maternal health for all women.
See Also
- [Paper] A Simulation-Based Comparative Effectiveness Analysis of Policies to Improve Global Maternal Health Outcomes (2023)
- [Paper] Assessing Differences in Country-Level Estimates of Maternal Mortality: A Comparison of GMatH, UN, and GBD Model Results for 2020 (2025)
- [Paper] Building an International Consortium for Tracking Coronavirus Health Status (2020)
- [Paper] Evaluating COVID-19 Public Health Messaging in Italy: Self-Reported Compliance and Growing Mental Health Concerns (2020)
- [Paper] Population-Scale Longitudinal Mapping of COVID-19 Symptoms, Behaviour and Testing (2020)
- [Paper] Precision Mapping Child Undernutrition for Nearly 600,000 Inhabited Census Villages in India (2021)
- [Paper] Simulation-Based Estimates and Projections of Global, Regional and Country-Level Maternal Mortality by Cause, 1990–2050 (2023)
- [Paper] Survey Data and Human Computation for Improved Flu Tracking (2021)
